Trichomoniasis Symptoms & Treatment
Trichomoniasis is a common, curable sexually transmitted infection (STI) caused by a microscopic parasite called Trichomonas vaginalis.
Trichomoniasis can affect both men and women but is most common in women, and older women are more likely to be infected than younger women. According to the World Health Organisation (WHO), trichomoniasis affects 8.1% of women globally.
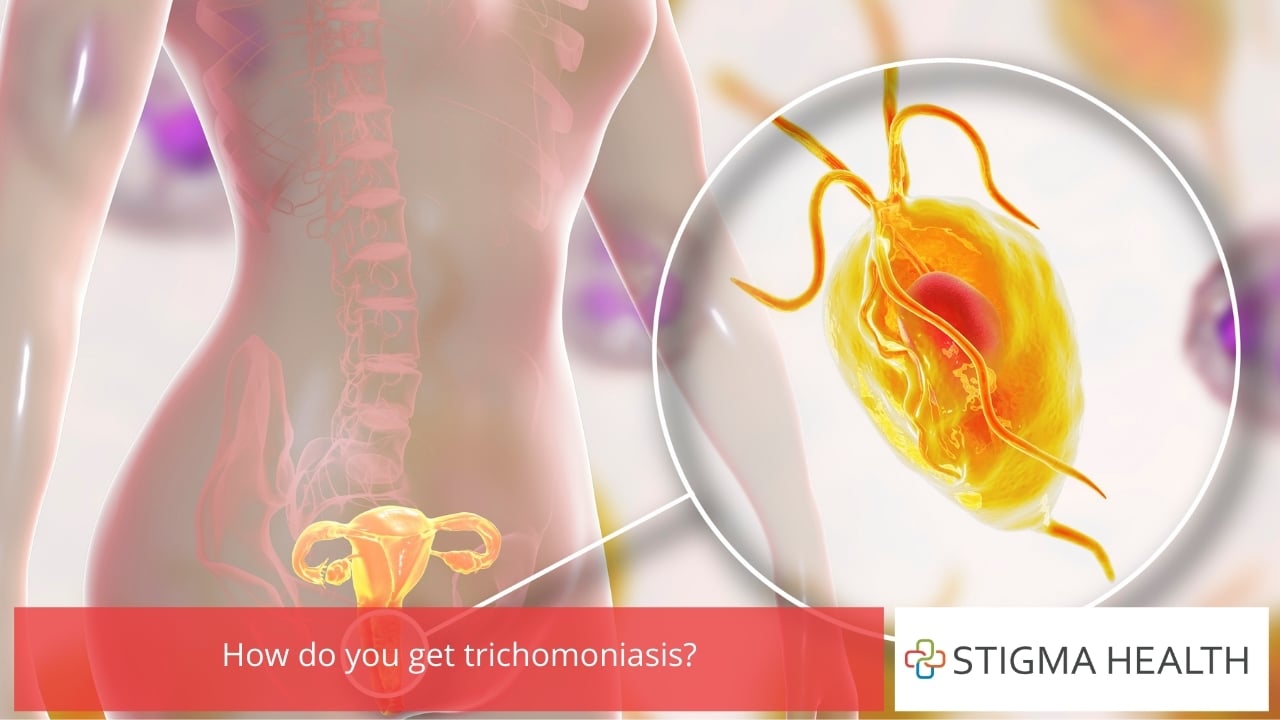
How do you get trichomoniasis?
Trichomoniasis is spread via unprotected genital contact, most commonly through intimate skin-to-skin or sexual contact, including vaginal, anal and oral sex – generally between a man and woman or between two women. It may also be possible for trichomoniasis to be spread through unprotected mutual masturbation (i.e., getting or giving a hand job, or fingering or being fingered) and sharing of sex toys.
Additionally, trichomoniasis thrives in damp conditions and there’s a slight possibility that it can be spread via public pools (if not cleaned thoroughly), sharing bath water, from a damp toilet seat, and from sharing damp personal items such as clothing, towels or washers.
What are the risk factors for getting trichomoniasis?
Risk factors for trichomoniasis infection include:
- Prior history of STIs
- Multiple sexual partners
- Work in the sex industry, or intimate or sexual contact with a sex worker
- Sex with a partner from outside Australia
- Low socioeconomic status
- Smoking
- Intravenous drug use
- Incarceration
- Residence in rural and remote areas (especially women), and in remote Aboriginal communities
Can you give trichomoniasis to someone else?
Absolutely! Trichomoniasis is highly contagious, and it doesn’t just affect the genitals – it can also infect the hands and mouth. It’s easily spread because up to 70% of people don’t have any symptoms, so it’s entirely possible to not know you’re infected and pass it on without realising.

What are the symptoms of trichomoniasis?
If symptoms of trichomoniasis appear, they usually show between 5 and 28 days after exposure, and may come and go. Symptoms can range from mild discomfort and irritation to severe pain and inflammation.
In men, trichomoniasis usually infects the urethra (tube your pee comes out of), but rarely produces any symptoms. When the infection does show symptoms they can include:
- swelling and redness around the head of the penis
- itching or irritation inside the penis
- pain or burning during urination or after ejaculation
- painful sex
- a white discharge from the penis
In women, trichomoniasis usually infects the lower genital tract, including the vulva (the outside of the vaginal lips), urethra, vagina and cervix (internal back wall of the vagina). Signs and symptoms include:
- redness, itching and burning, in and around the vagina
- pain or burning during urination
- lower abdominal pain
- painful sex
- a nasty smelling, thin (sometimes foamy) white, yellow, or greenish vaginal discharge
How is trichomoniasis diagnosed?
Your doctor may want to perform a physical examination – for women, this will likely include a pelvic exam – but conclusive diagnosis of trichomoniasis requires a pathology test. For women, a swab will likely be taken from the inside of the vagina, while men may be checked via a urine sample or swab from the opening of the urethra (pee hole).
Can trichomoniasis cause other problems?
Trichomoniasis infection can increase your risk of getting or passing on other STIs. For example, the genital inflammation caused by trichomoniasis can increase your risk of HIV infection or transmission, and women who have both HIV and trichomoniasis are more likely to pass on both STIs to their partners.
An untreated infection can potentially last for years and can lead to serious complications during pregnancy, including premature labour and low birth weight babies.

How is Trichomoniasis treated?
Unlike some other STIs, the body cannot clear itself of a trichomoniasis infection, so it needs to be treated with oral antibiotics. While a single large dose is often sufficient to treat most people, others may require a longer course in order to clear up the infection, and it often recurs – according to the CDC, around 20% of people will become re-infected within 3 months of being treated.
Antibiotics must be taken exactly as prescribed, to ensure they are as effective as possible, and you should wait at least a week after treatment is completed and all symptoms have cleared before you resume intimate or sexual contact with a partner. It’s recommended that you have a follow-up STI check 3 months after completing treatment to ensure the infection has fully resolved, however if your symptoms re-appear within this time you should get a check-up straight away.
If I have Trichomoniasis does my sexual partner need to be treated too?
If a diagnosis of trichomoniasis is confirmed, you and all of your sexual partners should be treated with antibiotics at the same time, to avoid re-infecting each other and prevent transmission to new partners. It’s important that everyone takes their medication exactly as prescribed, and that you all abstain from sex for at least 7 days after treatment is completed and symptoms have cleared.
How can I prevent Trichomoniasis?
The only truly effective means of prevention is to not have intimate skin-to-skin or sexual contact with another person. If you are sexually active the standard STI prevention strategies apply:
- always practice safe sex – use barrier protection (male or female condom, dental dam, or latex or nitrile glove/s) and a water-based lubricant every time you have intimate or sexual contact
- limit your number of sexual partners
- have an open and honest discussion about safe sex and your respective sexual health and sexual histories before you become intimate with any new sexual partner
- get regular STI tests
- seek treatment for any STIs you have

When should I see a doctor?
If you think you may have trichomoniasis, or you have any of the symptoms listed above, it is important to visit your doctor as soon as possible for diagnosis and treatment. Once a diagnosis has been confirmed, treatment is quick and easy.
See a healthcare professional as soon as possible if you think you or your sexual partner/s may have been exposed to an STI, or contact Stigma Health today to get tested.
References:
- https://www.cdc.gov/std/trichomonas/stdfact-trichomoniasis.htm
- https://www.healthdirect.gov.au/trichomoniasis
- https://www.healthline.com/health/how-can-you-get-trichomoniasis-if-no-one-cheats
- https://www.health.gov.au/resources/pregnancy-care-guidelines/part-g-targeted-maternal-health-tests/trichomoniasis
- https://pubmed.ncbi.nlm.nih.gov/21371384
