Hepatitis B Testing
Hepatitis B is a serious viral infection that affects the liver. It often goes unnoticed, yet it can cause long-term complications like cirrhosis and other liver diseases. The good news? It’s preventable, manageable, and easy to test for — especially with Stigma Health.
At Stigma Health, we remove the barriers that stop people from getting tested. No GP visit required. No awkward conversations. Just quick, simple access to a hepatitis B test through our online referral system. You choose your nearest pathology centre, and we deliver your results securely to your inbox or phone.
Get tested today or contact our friendly team for more information.
What is hepatitis B?
Hepatitis B is caused by the hepatitis B virus (HBV), a blood-borne virus that targets the liver and can cause both acute hepatitis (short-term infection) and, in some cases, chronic HBV infection — a long-lasting condition that may lead to serious liver disease.
Although hepatitis B is preventable with a vaccine and treatable with antiviral medication, it still poses a major public health challenge in Australia. In 2017, more than 233,000 people were living with chronic hepatitis B in Australia, and over 450 people died due to complications related to the infection (2).
Thanks to routine childhood immunisation and public health initiatives, notification rates among people aged 15–29 have decreased significantly. However, Aboriginal and Torres Strait Islander people, migrants from countries with high HBV prevalence, and people who inject drugs remain at higher risk of infection and underdiagnosis.
How is hepatitis B transmitted?
The hepatitis B virus is highly infectious — up to 100 times more infectious than HIV — and spreads through contact with infected blood or bodily fluids. This can happen through:
- Unprotected sexual contact with someone who has hepatitis B
- Sharing needles or injecting equipment
- Tattoos or piercings done with unsterile equipment
- Needlestick injuries (e.g. healthcare workers)
- From parent to child during childbirth (a major source of infection globally)
Most people living with chronic hepatitis B in Australia were born overseas and contracted the infection at birth or in early childhood — long before symptoms appeared. That’s why regular screening is essential, even if you feel completely healthy.

Who is at risk of hepatitis B?
You may be at increased risk of hepatitis B if you:
- Have ever had unprotected sex with a partner whose hepatitis B status is unknown
- Live with or have had close contact with someone who has chronic HBV infection
- Share personal items like razors or toothbrushes with others
- Inject drugs or have a history of drug use
- Work in a healthcare, prison, or childcare setting
- Were born in or have travelled to regions where hepatitis B is common, including parts of Asia, the Pacific Islands, and sub-Saharan Africa
- Are part of an Aboriginal and Torres Strait Islander community
- Are pregnant (hepatitis B screening is part of routine antenatal care)
If you’re unsure, getting a hep B test is the easiest way to check your hepatitis B status. And with Stigma Health, you can do it discreetly and on your own terms. Get tested today.
What are the symptoms of hepatitis B?
Many people with hepatitis B — especially in the early stages — won’t experience any symptoms at all. That’s why it’s often called a “silent” infection. When symptoms do appear, they typically include:
- Fatigue
- Fever
- Loss of appetite
- Nausea or vomiting
- Abdominal pain
- Joint pain
- Dark urine
- Pale stools
- Jaundice (yellowing of the skin or eyes)
These signs are often linked to acute HBV infection, which may resolve on its own. However, if the virus remains in the body for more than six months, it’s considered a chronic infection — and that’s when complications like cirrhosis or liver cancer can develop, often without any warning.
Experiencing hepatitis B symptoms? Don’t wait. If you believe you’ve been exposed to hepatitis B in the last 72 hours, visit your GP, a hospital or a specialty clinic ASAP to receive preventative post-exposure prophylaxis (PEP). For any other concerns, contact our team or book an STI test today.


What happens if hepatitis B is left untreated?
If hepatitis B isn’t diagnosed and monitored, it can silently damage the liver over time — even if you have no symptoms. People with chronic HBV infection are at significantly higher risk of developing:
- Liver cirrhosis (scarring of the liver)
- Liver cancer (particularly hepatocellular carcinoma)
- Liver failure requiring transplantation
Without early intervention, the virus can lead to irreversible liver disease, especially in people with additional risk factors like:
- Family history of liver cancer
- Age over 40
- Being assigned male at birth
- Smoking or high alcohol consumption
- Co-infection with hepatitis C, HIV, or other infections
- Conditions like diabetes or metabolic syndrome
The longer hepatitis B goes untreated, the greater the potential for serious complications. That’s why testing hepatitis B early is essential — even if you feel fine.
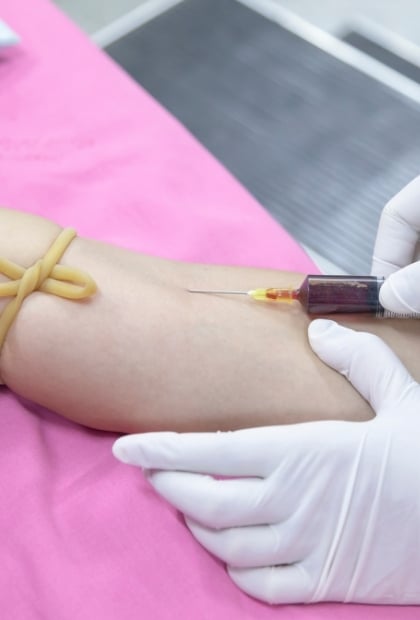
How do you test for hepatitis B?
A blood test is the only way to accurately diagnose hepatitis B. At Stigma Health, you can order your test online, attend your preferred pathology centre, and receive secure results — no GP visit or clinic appointment required.
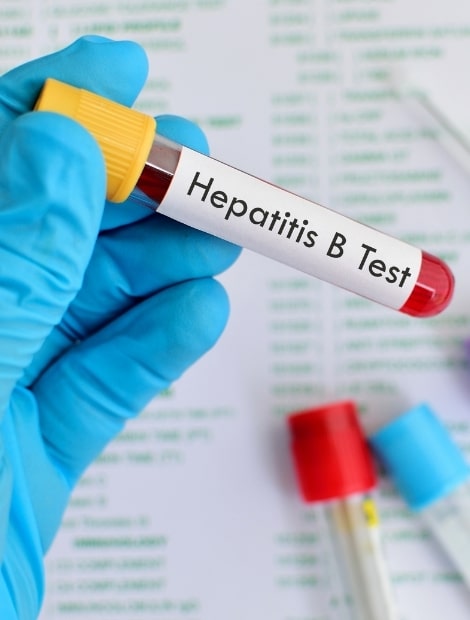
Our standard hepatitis B blood tests check for key markers, including:
- Hepatitis B surface antigen (HBsAg) — This indicates if you currently have the virus.
- Hepatitis B core antibody (anti-HBc) — This shows if you’ve ever been infected in the past.
- Hepatitis B surface antibody (anti-HBs) — This confirms whether you’re immune — either from recovery or the hepatitis B vaccine.
If needed, further testing may also include HBV DNA (to measure viral load) or liver enzyme levels (e.g. ALT, AST) to assess liver function. All of this can be done through simple hepatitis B blood tests at your local pathology collection centre.
Don’t wait — get tested today.
What does the hepatitis B vaccine do?
The hepatitis B vaccine is safe, effective, and the best way to protect yourself from the virus. It’s part of the National Immunisation Program in Australia and recommended for:
- All infants and young children
- People at higher risk (including healthcare workers, people who inject drugs, and people with multiple sexual partners)
- People with close contact with someone with chronic hepatitis B
- Travellers heading to regions with high HBV rates
- Aboriginal and Torres Strait Islander communities, where the burden of hepatitis B has historically been higher
The vaccine is delivered in a series of injections, typically over six months. Once you’ve had the full course, you’re considered immune — and protected for life in most cases.
You can check your hepatitis B status with a blood test to see if you already have immunity (via surface antibody) or if vaccination is recommended.
The bottom line on hepatitis B
Hepatitis B is more common than many people realise — and it often goes undetected. But with regular screening, it’s completely manageable. You can’t control when or where you were exposed, but you can take charge of your health now.
With Stigma Health, it’s never been easier to get a hep B test. You can:
- Order online without visiting a doctor
- Choose from 10,000+ pathology locations
- Get confidential results fast
- Access follow-up care if needed
No shame. No stress. Just straightforward testing you can trust. Get a hassle-free test today with Stigma Health.
References
- Peters MG. Hepatitis B Virus Infection: What Is Current and New. Top Antivir Med. 2019;26(4):112-116.
- Kirby.unsw.edu.au. 2019. HIV, Viral Hepatitis And Sexually Transmissible Infections In Australia: Annual Surveillance Report 2018 | UNSW – The Kirby Institute For Infection And Immun ity In Society. [online] Available at: <https://kirby.unsw.edu.au/report/hiv-viral-hepatitis-and-sexually-transmissible-infections-australia-annual-surveillance> [Accessed 4 August 2020].
- Krajden M, McNabb G, Petric M. The laboratory diagnosis of hepatitis B virus. Can J Infect Dis Med Microbiol. 2005;16(2):65-72. doi:10.1155/2005/450574
- Liang TJ. Hepatitis B: the virus and disease. Hepatology. 2009;49(5 Suppl):S13-S21. doi:10.1002/hep.22881
- Johan Westin, Soo Aleman, Maria Castedal, Ann-Sofi Duberg, Anders Eilard, Björn Fischler, Christian Kampmann, Karin Lindahl, Magnus Lindh, Gunnar Norkrans, Stephan Stenmark, Ola Weiland & Rune Wejstål (2020) Management of hepatitis B virus infection, updated Swedish guidelines, Infectious Diseases, 52:1, 1-22
- Australian Government Department of Health. Second national hepatitis B strategy 2014-2017. Canberra: Department of Health; 2014.
- Ashm.org.au.2012. [online] Available at: <https://ashm.org.au/resources/Hep_B_and_Primary_Care.pdf> [Accessed 19 August 2020].
- User, S., 2017. Hepatitis B – Australian STI Management Guidelines. [online] Sti.guidelines.org.au. Available at: <http://www.sti.guidelines.org.au/sexually-transmissible-infections/hepatitis-b> [Accessed 19 August 2020].
FAQs about hepatitis B
Hepatitis B is a virus that affects the liver. It spreads through infected blood or bodily fluids and can cause either a short-term (acute hepatitis) or long-term (chronic HBV infection). While some people recover completely, others may develop lasting complications like liver disease or liver cancer. A hepatitis B test is the only way to know your status.
A simple blood test can identify whether you currently have Hepatitis B, have had it in the past, or are immune due to the Hepatitis B vaccine. Your Stigma Health pathology referral will check for key markers like:
Testing is easy, fast, and available Australia-wide through our online system. Get your test today. |
Just follow these simple steps:
- Order your Hep B test through our website.
- Visit a local collection centre at a time that suits you.
- Get your test results delivered securely via SMS or email.
No appointments. No awkward chats. No fuss.
Yes. If the Hepatitis B virus stays in your body for more than six months, you’re considered to have chronic Hepatitis B. This can lead to liver damage, cirrhosis, and even liver cancer if left untreated. Regular testing and monitoring help manage this risk.
If you’ve had a past HBV infection and recovered, your body should have developed immunity. A surface antibody will usually appear on your blood test, confirming this. Reinfection is extremely rare but could be possible if your immune system becomes severely weakened or if you didn’t develop lasting immunity.
It depends on your risk level. If you have ongoing exposure (e.g. through work, travel, or sexual activity), or if you live with someone who has chronic hepatitis B, regular testing is recommended. Talk to your doctor or Stigma Health for personalised advice.
No. While both affect the liver, Hepatitis B and Hepatitis C are caused by different viruses and behave differently in the body. Both can lead to chronic infection, but they require different types of treatment and monitoring.
There’s no cure for Hepatitis B, but antiviral medication can help manage chronic Hepatitis B and protect your liver from further damage. In the early stages of acute HBV infection, most people recover without treatment, but monitoring is important.
f you believe you’ve been exposed to hepatitis B within the last 72 hours (e.g. via unprotected sex, needle stick, or blood contact), seek medical care immediately. You may be eligible for post-exposure prophylaxis (PEP), which can prevent infection if given early.
Get Judgement FREE Test
IMPORTANT: If you believe you may have been exposed to Hepatitis B in the last 72 hours do not proceed with a normal STI test, visit a doctor, hospital or specialty clinic ASAP so you can receive preventative post-exposure prophylaxis (PEP).
